Article – The outbreak hit fast last September, affecting fifteen children at several Calgary daycares. Parents panicked. Health officials scrambled to respond. But something different happened this time that could change how we handle these crises moving forward.
Researchers just published findings showing our city’s public health system caught this E. coli outbreak days earlier than traditional methods would have. That head start likely prevented more kids from getting sick. It’s the kind of quiet success story that doesn’t make big headlines but matters enormously to families across Calgary.
I’ve covered plenty of health scares over my years reporting in this city. This one stands out because of how detection worked. The usual approach involves waiting for doctors to notice patterns and report them manually. That takes time. Kids keep getting exposed while officials connect the dots.
Alberta’s health surveillance system used something called syndromic surveillance during this outbreak. The technology monitors emergency room visits and unusual symptom clusters in real time. When several children showed up with similar gastrointestinal problems, algorithms flagged the pattern immediately. Public health nurses investigated before the situation spiraled.
Dr. Jia Hu from the University of Calgary led the research team examining what happened. His study compared how quickly syndromic surveillance identified the outbreak versus traditional reporting methods. The results showed detection came roughly three days sooner with the digital monitoring approach.
Three days doesn’t sound like much until you consider how bacterial infections spread in daycare settings. Toddlers share toys, food, and close spaces. They’re not exactly known for stellar hand hygiene. Every hour counts when you’re trying to contain transmission among vulnerable populations.
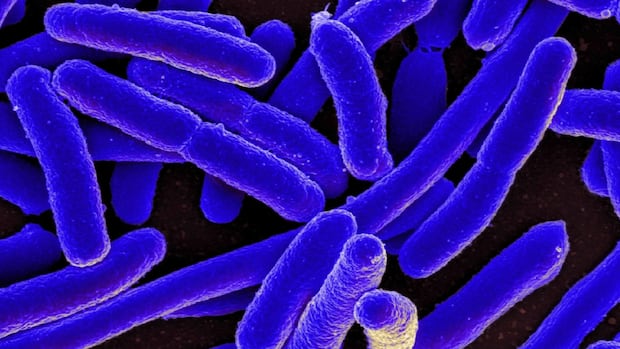
The study tracked fifteen confirmed cases across multiple childcare facilities in Calgary. All the affected children were under five years old. Several required hospitalization due to severe symptoms associated with Shiga toxin-producing E. coli. That particular strain causes bloody diarrhea and can lead to kidney failure in young children.
Alberta Health Services connected the cases to environmental contamination at the daycare facilities. Investigators never pinpointed an exact source, which happens more often than people realize with these outbreaks. But early detection allowed officials to implement control measures quickly. They closed affected classrooms, tested symptomatic children, and educated parents about warning signs.
I spoke with parents during the outbreak last fall. The fear was real and raw. One mother told me she felt helpless watching her three-year-old suffer through painful stomach cramps. Another father described the guilt of wondering if he’d somehow caused his daughter’s illness. These weren’t abstract statistics. They were Calgary families going through hell.
What struck me then and still does now is how much worse things could have been. Without early detection, more children would have been exposed before anyone realized something serious was happening. More families would have faced those emergency room visits and anxious nights.
The syndromic surveillance system Alberta uses pulls data from various healthcare touchpoints across the province. Emergency departments feed information continuously. The software analyzes patterns looking for anomalies that might indicate outbreaks. When thresholds get triggered, public health teams receive automatic alerts.
This technology isn’t new globally, but its effectiveness varies depending on implementation. Dr. Hu’s research specifically examined how well it worked in Calgary’s context. The findings suggest our local application deserves recognition and potentially wider adoption.
Traditional disease reporting relies heavily on laboratory confirmations and physician notifications. A parent takes their sick child to the doctor. The doctor orders tests. Labs process samples and identify pathogens. Results get reported to public health authorities. Each step adds delays.
Syndromic surveillance jumps ahead by tracking symptoms before definitive diagnoses exist. The system notices when unusually many children show up with severe diarrhea in a concentrated area. That pattern triggers investigation even while lab results are still pending.
Critics sometimes worry about false alarms with this approach. Computer systems might flag normal variation as potential outbreaks. Public health teams could waste resources chasing phantom threats. Dr. Hu’s study addressed those concerns by demonstrating the alerts led to genuine outbreak identification without excessive false positives.
Calgary’s experience offers lessons for other jurisdictions considering similar surveillance enhancements. The upfront technology investment pays dividends when it prevents even one severe outbreak from expanding. Hospitalization costs alone justify the expense, not to mention the human suffering avoided.
I’ve watched Calgary’s public health infrastructure evolve significantly over nearly two decades covering this beat. We’ve faced pandemic influenza, hepatitis outbreaks, and waterborne illness scares. Each crisis teaches lessons that improve our preparedness. This E. coli situation represents another step forward in that ongoing evolution.
The study also highlighted collaboration between multiple agencies during the outbreak response. Alberta Health Services, Alberta Health, and Calgary’s community health centers coordinated seamlessly. Information flowed quickly between organizations. That integration matters as much as any technological tool.
Parents deserve to know their children attend facilities monitored by these advanced systems. Daycare operators benefit from faster public health support when problems emerge. The entire community gains protection through improved disease surveillance capabilities.
Moving forward, researchers want to refine the algorithms further. Machine learning could potentially identify outbreak patterns even earlier. Integration with additional data sources might enhance detection sensitivity. The technology will keep improving as we learn from each real-world application.
What happened last September wasn’t just about fifteen sick children and worried families. It demonstrated how smart investment in public health infrastructure protects all of us. Early detection systems represent the kind of unsexy but crucial capability that separates good health systems from great ones.
Calgary continues building resilience against future threats. This study confirms we’re heading in the right direction. The next outbreak will come eventually. When it does, we’ll be better prepared to catch it quickly and protect our most vulnerable residents.